Leadup – Where do I start. Sort of crazy last few days. Guess it all started with a uncharacteristic cough on Sunday night which naturally worried Mom and Dad since I have CF and we never want me to get sick. Then on Tuesday, Mom went to Dallas for training on some new software so it was just me and Dad and we were hoping to watch the Capitals continue their hot streak in hockey and get some rest. Instead, I just couldn’t get comfortable and kept waking up Dad (more like not letting him go to sleep) so he contacted Children’s National. Upon explaining the symptoms to the on-call Pulmonologist, the suggestion was simple – “Bring Jack in and let’s take a look at him.”
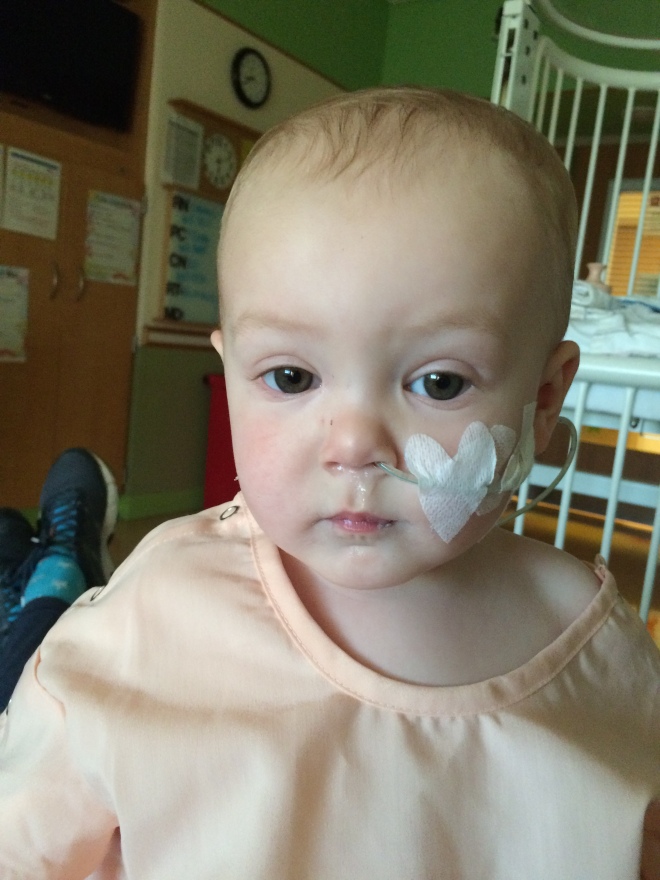
TUES: Upon Immediate Arrival – So Dad loads me up in the car and we head to Children’s at 12 midnight. The good news about heading to the ER at midnight is there is no traffic getting there and usually isn’t much of a line so we were seen within 15 minutes and headed straight back to an ER room. We then waited for hours until a room was available on the Pulmonary wing of the hospital (9:00 AM). This whole time Dad never told Mom we were heading at the hospital. He dodged FaceTime calls and everything to avoid worrying Mom who was many miles away. Mom is not very happy about this. Expect some changes around the Peden household as it relates to information sharing.
The symptoms which Dad felt were necessary to bring me in were actually warranted – slight fever, hard and distended abdomen, lack of appetite and no stooling. Dad’s heart was sinking. We had just left Children’s about a month ago for what was a small blockage and Mom was out of town. The ER nurse hooked me up to and IV sent me off to X-Ray.
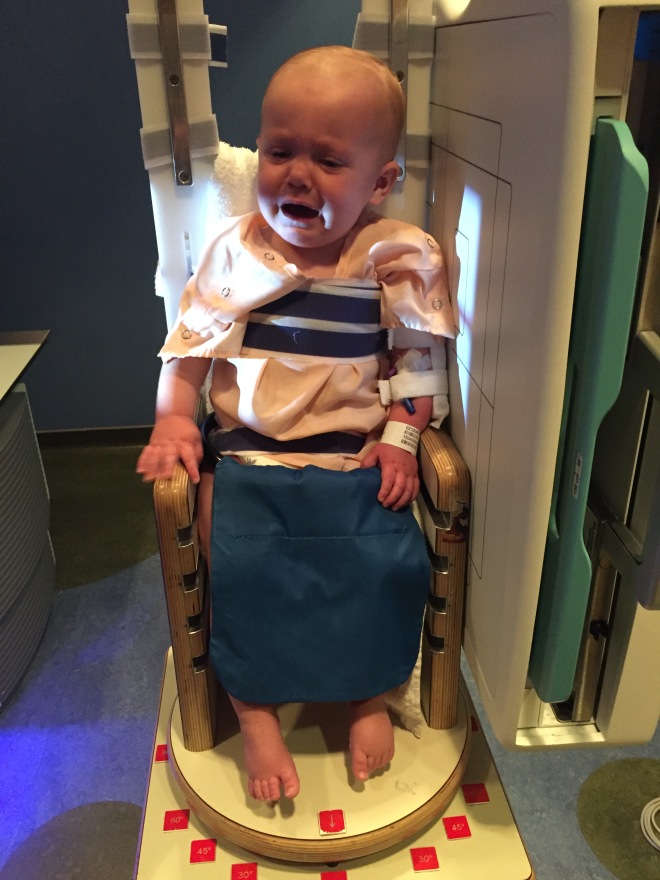
Above, is where I am getting ready for my first X-Ray this stay. Dad said it reminds him of Peter Quinn in a recent episode from the hit show Homeland. Dad wondered what it would be like to send this photo to mom who was still 1340 miles away. He thought better of it and opted to simply text sweet messages about how perfect I am.
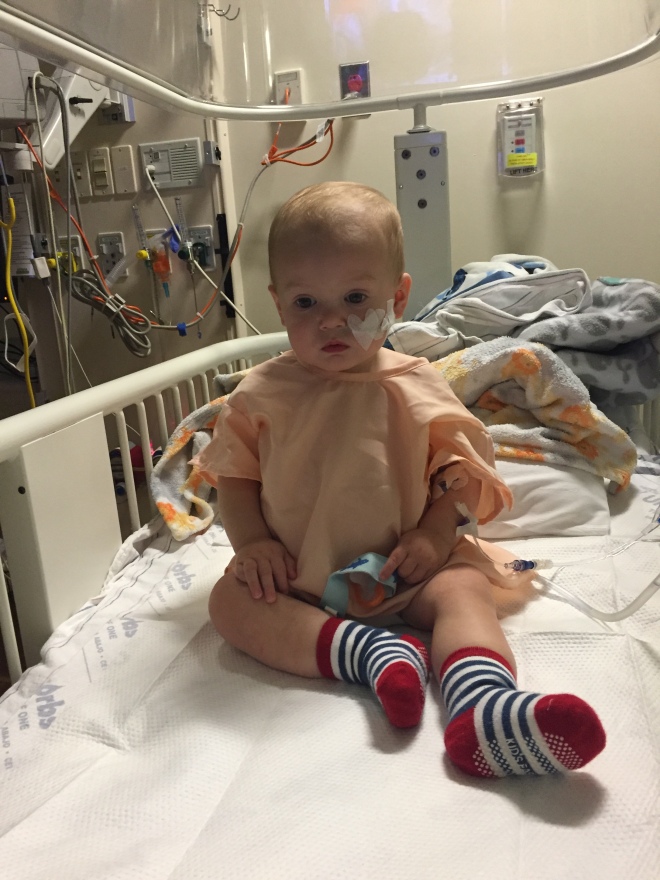
WEDS: Off to Pulmonary – After four X-Rays, an IV, and a NG tube…we headed up to Pulmonary where were finally examined by the specialists. Naturally, they were concerned as to why I was back so soon and wanted to get to the bottom of it and Mom began to become concerned as to why Dad was ignoring FaceTime calls so then Dad answered and holy s***, you would have thought Mom slammed her fingers in a car door. She immediately left the breakfast table and began sobbing on the video – exactly what Dad hoped to avoid. So Mom sat through half of training, changed her flight and headed home early…arriving to the hospital at about 10:30 PM. From a medical perspective they kept me hooked up to the IV for continued fluids and an intermittent sump (suck) on my NG tube to try and suppress the distention in my bowels. They also pumped 800 mL of GoLytely through my NG tube in hopes to soften up any stool which was causing a blockage.
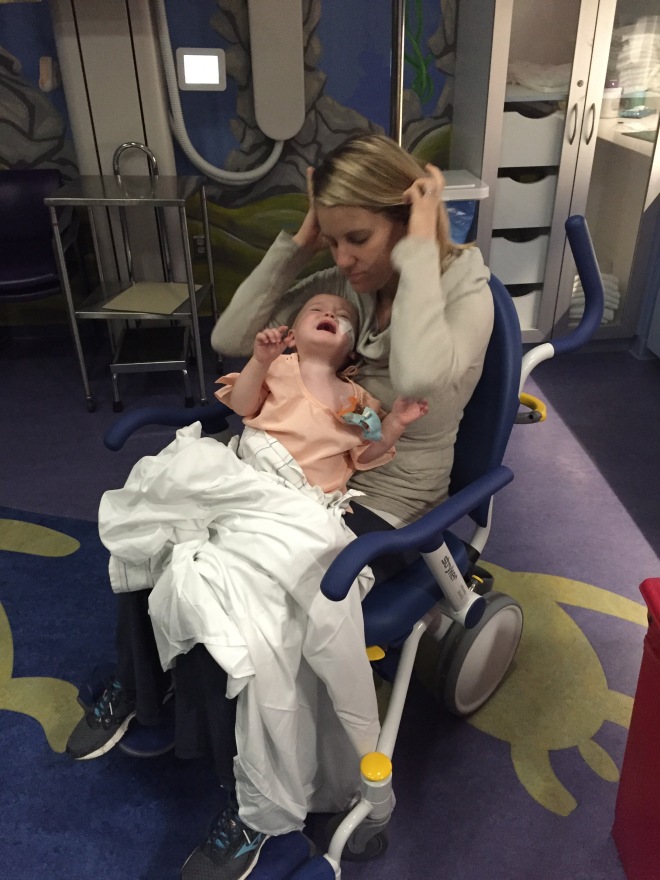
THURS: Enema #1 – Oh sweet, more enemas. Not really. Since the sump wasn’t doing too much and my distention or comfort level hadn’t improved much at all, this was the next procedure to try. For anyone who hasn’t had an enema, let me just say…they are not fun and if you don’t believe me, I highly encourage you to listen to a fellow CF’er, who takes a humorous approach to an enema he had as a teenage boy. You can listen to it here – Sickboy Podcast.
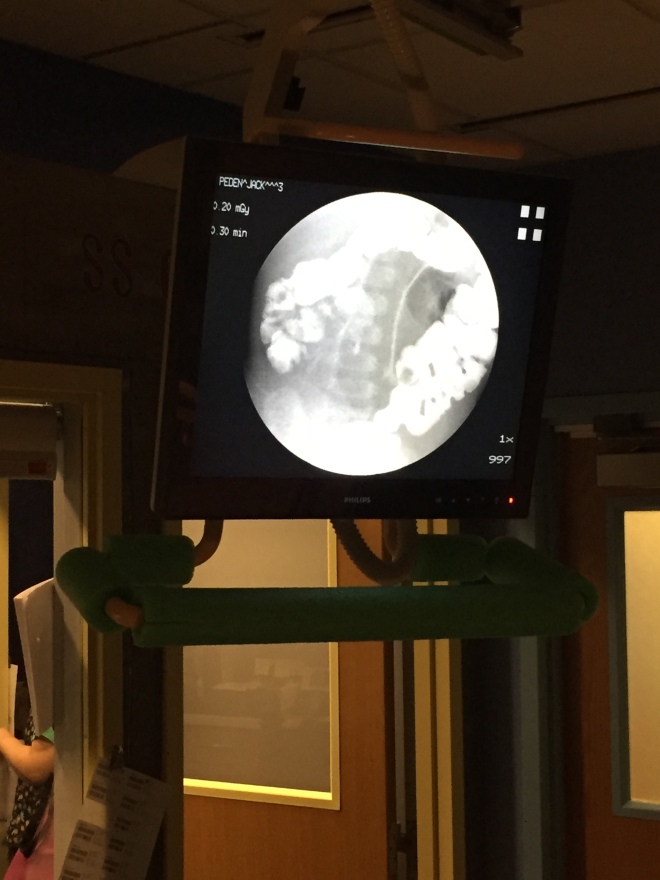
In this photo, the contrast successfully made its way from my colon and large bowels, but stopped right along the area where it joins up with the small bowel.

While this enema gave us some hope, it’s still concerning. The team of surgeons felt we should try Mucomyst down my NG tube and would try another enema in the morning. My abdomen continued to grow even with suction on my NG tube.
FRI: Enema #2 – At about 3:00 AM Friday, I began to vomit up the Mucomyst that was inserted into my NG tube which wasn’t good as that was a sign that this block likely wasn’t going away like last time. It also meant the enema was the only chance to avoid surgery. At 9:00 AM Friday, Dr. Sami rushed me down to the radiology department to get me in right away. The doctors opted to include Mucomyst in my enema this time around hoping to penetrate the blockage and loosen it up. Humans would be shocked at how much fluid one could shoot up one’s colon into their bowels. At any rate, this didn’t work and the contrast actually didn’t make it as far as the day previously so Radiology, Surgery, Pulmonary, and everyone else weighed in on what to do next.
Surgery – Without much hesitation, everyone felt surgery was necessary so it was back under the knife since day two of birth. At 2:15, they put me under, while Mom, Dad, Rachel, and Pop waited upstairs. After about two hours, the surgeons came out to give Mom and Dad the news.
While surgery is never good, this surgery was as favorable as surgery could be, given the options that were on the table. Cutting along my previous incision, surgeons began to pull out my small bowels. They quickly noticed that my small bowels had adhesions, likely from the previous surgery that was completed to correct my Meconium Ileus (MI). Anytime the bowels are cut or touched, adhesions are not uncommon. Abdominal adhesions are difficult to predict and do not show in imagery so this wasn’t something that had been discussed with Mom and Dad. All Mom and Dad were told is that the exploratory surgery would lead to any number of things – removing part of my small bowels, an ostomy bag, etc. Surgeons worked quickly to remove the adhesions and straighten out the small bowels where they seemed to have “corkscrewed” right at the Ileum. Given its location along the bowels, the Ileum is the most difficult area to get to and work on which is another reason surgery was practically unavoidable at this point. After my bowels were pulled out, they sucked out all remaining fecal matter through my NG tube and felt there were no signs of Meconium in my small bowels so they did not need to cut along my bowels again. Because the small bowels did not need to be cut open, this was great news. In a way, it means that my mechanical workings of my bowels appear to be operating properly, but the adhesions were the likely cause of the problem. As such this was not a direct correlation to CF, but more-so of my previous surgery (which was due to CF).
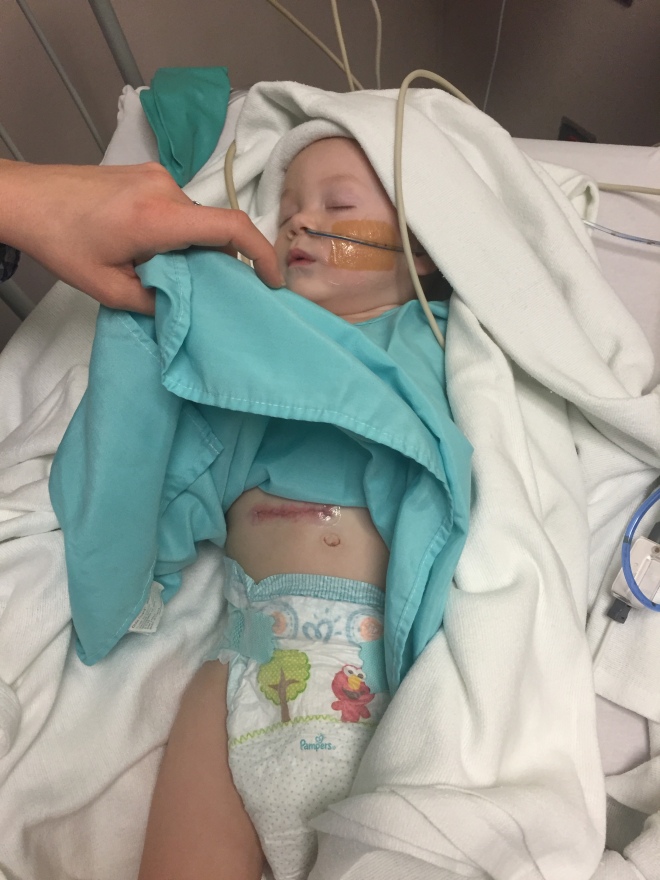
Sat: On the Mend – My team here at Children’s reassured the other half of Team Jack that there was nothing they could have done to prevent this and that they have been doing a great job thus far. Abdominal adhesions are just a thing that is more common in individuals who’ve had some sort of abdominal procedure (i.e. Appendectomy).
This stint at Children’s should serve as a friendly reminder to Team Jack and others that we have to be extra careful this holiday season and do our best to keep me away from people that are sick or might be sick. We all must do a good job at cleaning everything thoroughly to reduce my exposure to germs. Also, anyone picking me up or holding me…shall be very careful not to pick me up by my arms/underarms/etc as that will pull on the incision and other areas of the abdomen which are incredibly tender and sore.
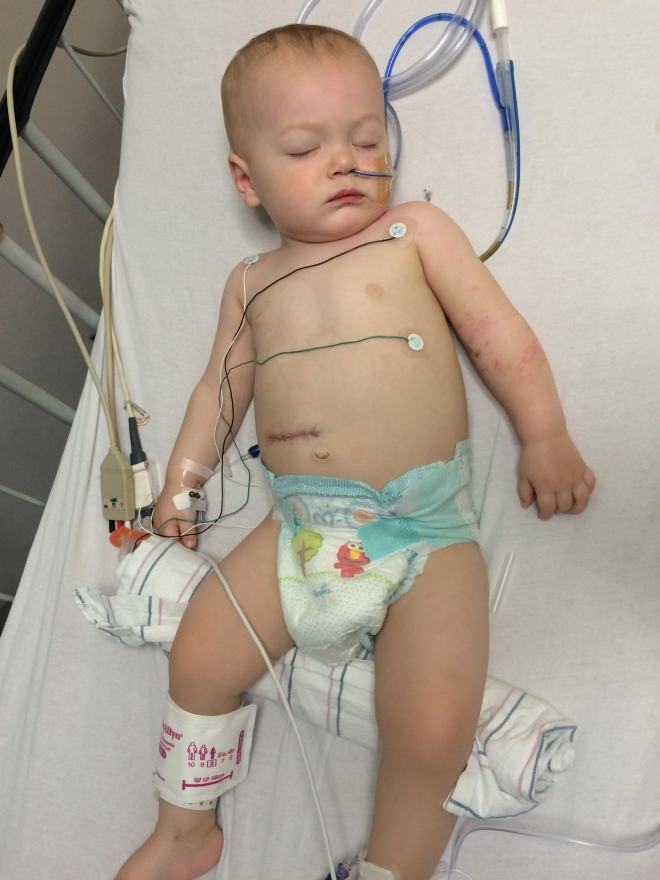
Thanks everyone for the well wishes and to all of those checking in on me. I’m determined to not let this slow down my ability to full out walk. I was making good progress just prior to this incident so while I’ll be sore, this isn’t going to hold me back. I’ve already begun pulling myself up on the crib rails. Hoping to get out of here before Christmas (maybe as little as one week).






















